Laser cataract surgery is a newer and more technologically advanced method of removing cataracts compared to traditional cataract surgery. During laser cataract surgery, a femtosecond laser is used to make precise incisions and remove the cloudy natural lens in the eye. The benefits of laser cataract surgery include:
- More accurate incisions, resulting in less induced astigmatism and faster vision recovery1
- More precise capsulotomy, allowing for optimal positioning and centering of the artificial lens implant2
- Potentially less ultrasound energy used during the procedure
- Possibly safer outcomes for patients with certain eye issues like weak corneas
While promising, laser cataract surgery is still an emerging technology. Its higher costs and lack of long-term clinical data have limited insurance coverage so far.
High Upfront Costs
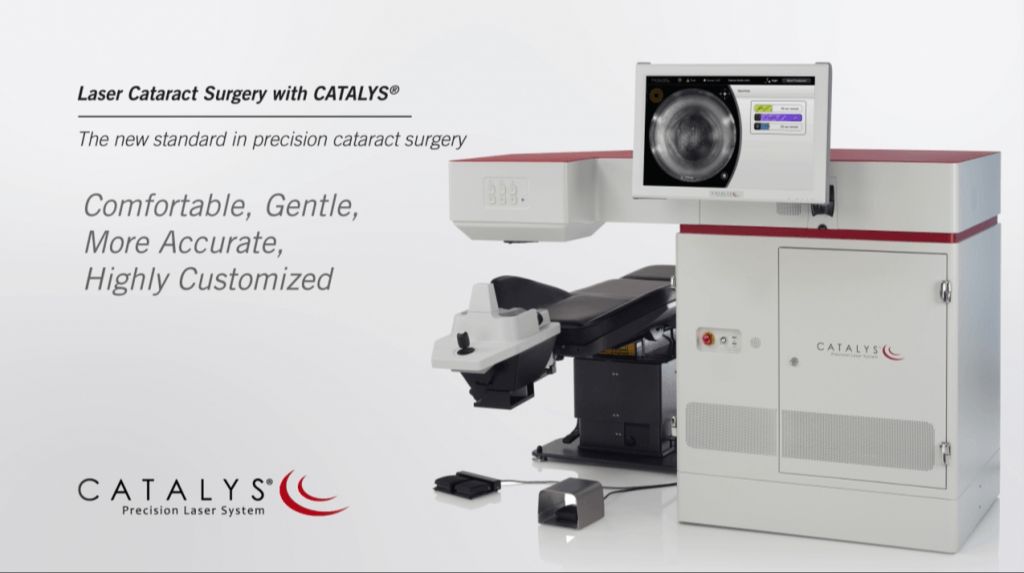
Laser cataract surgery systems involve a high upfront investment for ophthalmology clinics and practices. According to sources, the femtosecond laser units themselves cost approximately $400,000 to $500,000 to acquire initially [1][2]. This substantial capital expenditure is often prohibitive, especially for smaller clinics. Additionally, there is an ongoing usage fee or “click” fee charged for the disposable components used during each procedure, further adding to costs.
Given the high acquisition and recurring costs, many practices cannot afford these expensive systems. As a result, insurance providers may be hesitant to cover laser cataract surgery until the technology becomes more widely adopted and accessible.
Lack of Long-Term Data
Laser cataract surgery is a relatively new procedure, having only been approved by the FDA in 2010. As a result, there is limited long-term data available on the outcomes and side effects compared to traditional cataract surgery.
A 2011 review found a lack of long-term clinical data on femtosecond laser systems used in cataract surgery. The authors stated “The final cost-benefit analysis will be more complete once long-term data on the laser systems is available.” [1]
A key question is how well laser cataract surgery maintains visual acuity over time. A 2016 Swedish study that followed patients for 15 years after traditional cataract surgery found visual acuity deteriorated over time. [2] More studies like this are needed to compare the long-term outcomes of laser versus traditional techniques.
Insurance providers are hesitant to cover a procedure without sufficient evidence that it provides better long-term results compared to standard treatment. While short-term data on laser cataract surgery is promising, insurers are awaiting more conclusive long-term studies before considering coverage.
Not Deemed Medically Necessary
One of the main reasons insurance companies won’t cover laser cataract surgery is because they don’t deem it “medically necessary.” Most insurance plans only cover treatment that is required to restore basic health and vision. They view laser cataract surgery as more of an elective procedure because it only provides incremental improvement beyond what is achievable with traditional cataract surgery.
While laser cataract surgery offers potential benefits like better vision, faster healing times, and more precise incisions, insurance companies argue that standard cataract surgery is sufficient for treating the medical condition. From their perspective, the added benefits of laser surgery are desirable but not absolutely essential. So they classify it as an elective upgrade rather than a medical necessity.
For insurance providers to cover a treatment, it needs to be the standard of care for diagnosing or treating a medical problem. Since traditional cataract surgery meets that standard, insurers can deny claims for laser cataract surgery even though many patients and surgeons feel it provides better outcomes.
Not Covered by Medicare
Medicare has not approved coverage for laser cataract surgery. According to the Centers for Medicare and Medicaid Services (CMS), “Under either method, Medicare will cover and pay for the cataract removal and insertion of a conventional intraocular lens” (CMS). This means that while Medicare will cover traditional cataract surgery, it does not cover the use of lasers. The laser portion of the surgery is considered an “upgrade” and beneficiaries must pay out of pocket if they want laser cataract surgery. Medicare views laser cataract surgery as an elective, non-covered service.
Considered Experimental
One key reason insurance companies are hesitant to cover laser cataract surgery is because it is still considered experimental and investigational by the FDA and insurance companies. While laser cataract surgery systems like Lensar and Ziemer have received FDA clearance in recent years, the long-term data and clinical trials demonstrating safety and efficacy over the traditional manual technique are still lacking.
According to the FDA, clearance means the devices have met the “reasonable assurance of safety and effectiveness” standard for market release, but does not imply official approval or that clinical benefit has been established (1). Insurance companies echo this sentiment, wanting to see more evidence and peer-reviewed studies before agreeing to take on the costs of the newer laser method.
Without FDA approval and recommendations from major medical societies, laser cataract surgery is deemed experimental by insurers. And experimental procedures are usually excluded from coverage (2). So until more data and trials convince the FDA and insurance companies of the benefits, laser cataract surgery is unlikely to be covered.
(1) https://www.fda.gov/patients/device-development-process/step-3-pathway-premarket-submission
(2) https://www.aao.org/education/headline/fda-approves-laser-refractive-cataract-surgery-2
Lacks Clinical Trials
While some small clinical studies have shown potential benefits of laser cataract surgery, large randomized controlled trials are still needed to definitively prove its advantages over traditional phacoemulsification cataract surgery. A 2020 randomized trial of 350 patients found no significant difference in visual acuity between laser and standard cataract surgery at 3 months post-op (Day et al.). Another randomized trial in 2021 of 242 patients also found laser cataract surgery to be non-inferior to conventional surgery in terms of visual acuity (Wang et al.).
Insurance providers are waiting on more substantial clinical evidence from large, multi-center randomized trials with long-term follow-up before considering coverage of laser cataract surgery. While early results are promising, laser technology for cataracts has not yet been proven through rigorous clinical trials to justify the higher costs compared to established standard surgery.
Seen as a Luxury
Laser cataract surgery is often perceived as an expensive elective upgrade rather than a medically necessary procedure. While traditional cataract surgery is usually covered by insurance, laser cataract surgery is viewed by many insurers as a luxury service.
The high upfront costs of laser cataract surgery, which can be $1000-$2000 more than traditional cataract surgery per eye, position it as a premium offering in the eyes of insurance companies. With alternatives available at lower costs that insurance does cover, laser cataract surgery is seen as an optional add-on service rather than a required procedure.
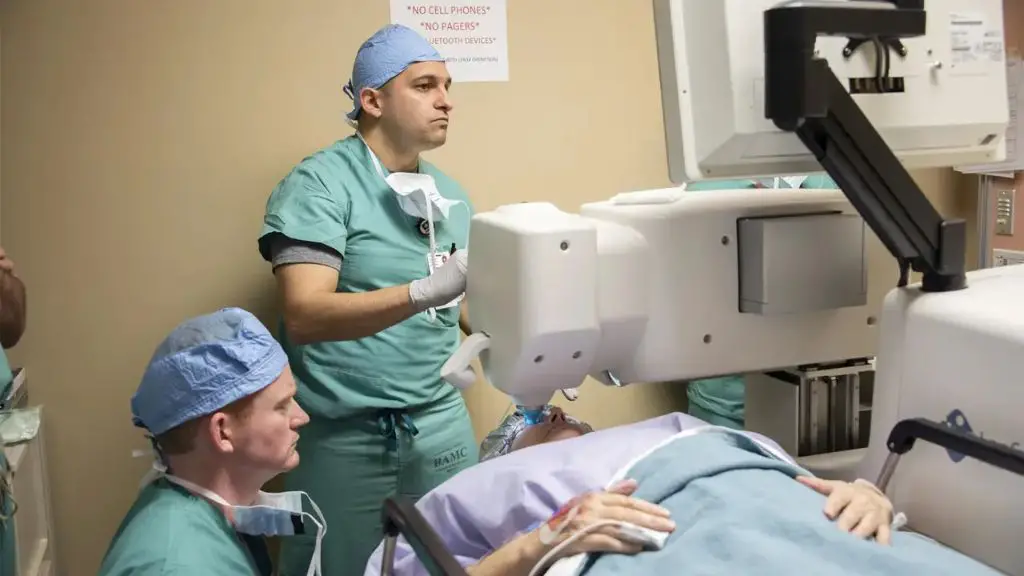
Some insurers view laser cataract surgery as a financial opportunity for surgeons to increase revenues by marketing a new technology, rather than a change that significantly improves patient outcomes. Without definitive clinical evidence of superior results, insurers are hesitant to take on the additional expense of covering laser cataract surgery.
Overall, the perception of laser cataract surgery is that it is a nice extra for those who can afford it, but not a necessity that insurance is obligated to cover. Positioning it as an elective luxury service limits insurance coverage for a procedure that proponents argue can improve precision and patient experiences. But unless perceptions shift, laser cataract surgery is likely to remain an out-of-pocket expense for most patients.
Alternatives Covered
Standard cataract surgery using traditional phacoemulsification is reliable and has been performed for decades. Phacoemulsification uses ultrasound waves to break up the cloudy lens and remove it through a small incision. This procedure is proven safe and effective, with over 3 million cataract surgeries performed each year in the U.S. alone.
Since traditional cataract surgery is well-established, insurance companies readily cover this procedure. Medicare and most health insurance plans classify standard cataract removal as medically necessary. The lower cost and widespread coverage make traditional phacoemulsification the default option covered by insurers.
Conclusion
In summary, insurance companies tend to exclude coverage for laser cataract surgery for several key reasons. The high upfront costs of the new laser technology make the procedure significantly more expensive than traditional cataract surgery. Insurance providers are hesitant to cover laser cataract surgery until more long-term data is available demonstrating improved patient outcomes over current methods. Medicare and many major insurance plans still consider laser cataract surgery experimental or investigational, rather than an accepted standard of care. Without large clinical trials, laser cataract surgery struggles to shed the perception that it is an elective, luxury procedure rather than a medical necessity. While the technology shows promise, the lack of clinical evidence and higher costs mean most insurance plans still favor covering traditional cataract surgery over newer laser techniques for the time being. However, as further research emerges and prices fall, coverage policies may continue to evolve.

